Disc Prolapse: Symptoms, Causes, Diagnosis, and Treatment

Key Highlights
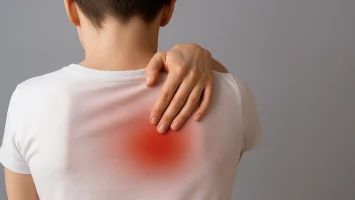
Disc prolapse, often called a herniated disc, is a common reason for back pain and nerve pain. This problem can make it hard for people to move as they usually do.
The issue mostly appears in the lower back, the neck, or the middle back, specifically in the lumbar, cervical, or thoracic spine. People may have lower back pain, feel pain in the neck, or notice sensory changes in the body.
To determine the right treatment, doctors use imaging tests such as MRI or CT scans. These help to know what is really happening in the back and where exactly the trouble is.
The ways to address this problem can vary. Some people will get better with non-surgical help, like physical therapy, but others with more severe problems might need surgery.
To reduce the risk of developing a herniated disc again, maintain good posture and engage in regular exercise. These steps are essential to maintaining a healthy back.
It is essential to recognize when symptoms worsen, such as experiencing weakness in the legs, experiencing sensory changes, or losing control over your bladder. Knowing about these signs early will help you get the right medical help faster, giving you the best chance for a good recovery.
Introduction
Having a herniated disc can be scary and very painful. This is true when you experience lower back pain that radiates down your legs or makes it difficult to move. A herniated disc happens when the soft middle part of an intervertebral disc breaks and presses on the spinal cord or nearby spinal nerves. When this occurs in your lower back, it can cause significant back pain and even impact your mobility. These problems need the right diagnosis and care to stop long-term harm. If you know what can cause this, the treatments that work, and ways for recovery, you get hope and real help for dealing with a herniated disc.
Understanding Disc Prolapse
Disc prolapse, also known as a herniated disc, occurs when the soft, central part of the intervertebral disc, called the nucleus pulposus, protrudes through its outer, tough layer. When this happens, it can bother or press on nearby nerves. That can cause pain, numbness, or even weakness. These discs are like cushions that sit between the bones of your spine. They help your back withstand the impact of movement and allow you to bend or turn. As people age, or if they experience repeated injuries or certain actions, the disc can become weak. This can make it easy for the disc to get hurt.
It is essential to understand how and why a herniated disc occurs if you want to manage your symptoms effectively. The lower back, also known as the lumbar spine, is most likely to experience a herniated disc because it carries the most weight for the body. Still, your neck (that’s the cervical part) and the middle of your back (thoracic area) can also have this issue. If you notice signs early and consult a doctor, you can help prevent further problems and find ways to maintain your spine’s health and mobility.
What is Disc Prolapse?
At its core, a herniated disk happens when the soft part in the middle of the disk, called the nucleus pulposus, pushes out through a tear in the tough outer layer, known as the annulus fibrosus. This tear lets some disc material escape. It can press on the spinal nerves or narrow the spinal canal. This sometimes causes pain or discomfort. People say that the pain can feel like burning or be sharp and may go down into their arms or legs.
A herniated disk can happen anywhere in your back, but it is most common in the lumbar spine or the neck. These areas move more and take on more stress. If the lumbar spine has a ruptured disk, the disc material may press on the sciatic nerve, giving sharp pain down the leg. With neck pain from a herniated disk in the neck, the pain may spread into the shoulder or down to the arm.
Not everyone with a herniated disc experiences symptoms immediately. Sometimes, a person discovers a herniated disk while undergoing scans for another condition. However, if you experience nerve symptoms, pain, or discomfort, seek medical help immediately. This is important to help prevent more nerve damage from happening.
Types of Disc Prolapse (Lumbar, Cervical, Thoracic)
Disc prolapse can occur in various parts of the spine. Each place can have its own kind of trouble. When a disc herniation occurs in the lower back, it is referred to as a lumbar disc herniation. This problem often brings lower back pain. It can also press on nerve roots, so the pain can travel down the legs.
If a disc prolapse occurs in the neck, you are likely to experience neck pain. It may also cause the pain to radiate down the arms. This is because the spinal nerves in that area can become compressed.
Thoracic disc prolapse is not as common. It can cause pain or soreness in the upper back. In more severe cases, it might even reach the point of affecting bowel control.
Knowing the difference between these types is very important. That way, people can get the right care for relief from back pain and discomfort.
Consult with top pain specialists in your city.
Key Symptoms of Disc Prolapse
Knowing the signs of disc prolapse is crucial for seeking help on time. Back pain, especially in the lower back, is usually the first thing people notice. It may start with some discomfort. Over time, this back pain can worsen and may become increasingly difficult to bear. When nerve root compression occurs, sensory changes may be present. People may feel tingling or numbness in some parts of their body.
In severe cases, more serious problems can occur. You may find that your legs become weaker, or you may experience problems with bowel or bladder control. These signs indicate that you need to seek medical attention immediately. If you know about these symptoms, you can tell the difference between disc prolapse and some other problems that affect your spine. This helps ensure you consider the right treatment options for lower back pain related to nerve root issues and other sensory changes.
Common Signs and Physical Manifestations
Disc prolapse can manifest in various ways throughout the body. It can progress from minor pain to significant trouble when moving around. Here are some common signs to look for:
- Low back pain: You may feel an ongoing pain in your lower back. It often worsens when you move or sit for a prolonged period.
- Muscle weakness: You could find it hard to lift things. Sometimes, your grip is not as firm as it used to be.
- Radiating leg pain: You may experience sharp or shooting pain that starts in your lower back and radiates down one leg.
- Straight leg raise test outcomes: If you lift the affected leg while lying flat and it hurts, it could mean that a nerve is irritated.
These signs can interfere with your day-to-day activities. That’s why it’s important to find the problem early. If the disc problem is in your lower back, you may experience leg pain that resembles sciatica. If it’s higher up in the neck, you could feel tingling or pain in the arm. The right tests, including the straight leg raise test and neurological checks, help doctors know which part of the back is causing the trouble. Receiving the correct diagnosis is crucial for effective relief.
Nerve-Related Symptoms
When a disc bulges out and presses on the spinal nerves, it can cause more than just simple pain. These nerves, when affected, bring on other clear problems such as:
- Sciatic nerve pain: This causes an intense, sharp pain that originates in the lower spine, extends through the buttocks, and can radiate down one leg.
- Cauda equina syndrome: Although rare, it is a very serious condition. It is caused by spinal cord compression and leads to issues with bladder or bowel control.
- Tingling and numbness: You may feel these kinds of sensory changes in certain nerve areas.
If nerve damage persists for too long, muscle strength may decline. This can make it hard to walk well or use your hands for simple things. If you show signs of cauda equina syndrome or anything this serious, it is very important to get help right away. Early treatment could help you avoid permanent problems from the loss of spinal cord function.
Causes and Risk Factors
Many things can cause a disc prolapse. These may be age-related changes in the body or problems with the spine itself. As we get older, the discs in our back go through wear and tear. This can bring on disc disease or even degenerative disc disease. These problems make it easier for a disc to move out of place.
Repeating the same activity over and over can increase the risk, especially if it is done incorrectly. Lifting heavy objects without proper care is often the cause. Harm or injury to your spine might also lead to trouble. This may cause nerve root compression. Then, you can experience pain that radiates down to the lower extremities, such as your legs. It is good to know what can cause disc prolapse. By learning about these risks, you or others can try to avoid them. Good habits and care help with both prevention and the right treatment.
Degenerative Changes and Aging
As the body gets older, the discs in the spine wear down. This can cause back pain, disc degeneration, or even chronic back pain. The nucleus pulposus, which is the soft, gel-like part in the middle of the disc, starts to lose water and is not as elastic as before. Because of this, the discs can’t absorb shock as well as they used to. This increases the likelihood of the discs breaking down and causing nerve root compression. When that happens, you may feel discomfort while doing your daily activities.
Being aware of the changes that come with age is important. They can significantly impact the health of your spine, the strength of your muscles, and the functioning of your nerve roots. These problems often make it hard to move and can cause pain as people age.
Injury, Trauma, and Repetitive Strain
Injuries and trauma, like heavy lifting or sudden falls, can cause a herniated disc. This issue can happen in both the lower back and neck parts of the spine. When this occurs, inflammation and nerve root compression may result. This often leads to ongoing back pain or neck pain. Repeating the same motions over and over again from daily activities, such as maintaining poor posture or sitting for extended periods, can also contribute to disc disease. Over the years, these habits can lead to degenerative disc disease. Knowing about these things is important. It helps people use effective methods to prevent back or neck problems, seek treatment when needed, and work to maintain the health of their spines, resulting in reduced discomfort.
How Disc Prolapse Develops
Changes in the intervertebral discs occur slowly due to factors such as aging and back pressure. As the years go by, the nucleus pulposus, which is in the center of each disc, can get weak. This causes the disc material to bend or shift out of place. Sometimes, there can be a herniation of the disc, which is called a disc herniation.
When this happens, it may press on nearby spinal nerves. People can start to experience low back pain or, if the nerve root is compressed, nerve root compression in the legs or lower back. It is important to see these signs early. Doing so may stop things from getting worse and help avoid strong back pain or other serious problems. Recognizing issues with the nucleus pulposus or any disc herniation can help prevent more significant problems with the spinal nerves later on.
Pathophysiology Explained
Disc prolapse occurs due to a combination of factors that are all interconnected. At first, the intervertebral disc, which is made up of the nucleus pulposus and the outer ring called the annulus fibrosus, starts to wear out. This can result from aging or performing the same movement repeatedly. When this part wears out, the outer ring of the disc gets weak. It then makes it easy for the disc material to push out.
When the disc material bulges out into the spinal canal, it may press on the nearby spinal nerves. This can cause a person to experience pain, muscle weakness, or a change in sensation in the lower extremities. It is essential to understand this process thoroughly. It helps doctors develop effective plans for managing and treating individuals experiencing these issues.
Stages of Disc Herniation
The stages of disc herniation can really change your daily life. This often begins with pain in one specific area, typically in the lower back or neck. As the herniated disc gets worse, this pain can go into your arms or legs. That is because the nerve root gets pressed. Over time, the pain can get stronger. You may also notice muscle weakness or sensory changes, like numbness. It is essential to recognize these symptoms early, allowing you to explore treatment options. If you wait too long, a chronic issue might develop.
Diagnosis of Disc Prolapse
To determine if someone has a disc prolapse, the doctor begins by discussing their medical history with them and collecting a detailed medical history. The doctor wants to know about conditions such as back pain, nerve root problems, or nerve root compression. During the visit, the doctor does a physical check. The straight-leg raise is one test that helps identify the location of pain and weakness.
Then, the doctor uses imaging tests. MRI scans are the imaging modality of choice. They show clear pictures of the spine and discs. These help the doctor see the problem better. For people in severe cases, the doctor may need to use a CT myelography. This test helps give the doctor more information. From all this, they ensure the patient receives the correct diagnosis and a plan that is best suited for their recovery.
Clinical Evaluation and Medical History
A thorough clinical evaluation and a clear medical history are essential to determine if someone has a disc prolapse. Individuals with this condition often experience back pain, neck pain, or leg pain. This requires doctors to perform a physical examination, such as the straight leg raise test, to determine if nerve root compression is present. It helps to know about a person’s past injuries, their lifestyle, and the severity of their symptoms. This information can show if they have disc degeneration or a herniated disc. Collecting all these details is crucial to creating an effective treatment plan. It helps reduce pain and gets people moving again.
Imaging Tests: MRI, CT Scan, and X-Ray
Using the right imaging tests is crucial when doctors need to determine if there is a disc prolapse. MRI is usually the imaging modality of choice. It provides clear images of soft tissues, such as the intervertebral disc and spinal nerves. CT scans are also helpful, especially for examining bones and identifying herniated discs. X-rays do not show as much about soft tissues. But they can still show if there are any changes in the spinal canal. These tests help doctors assess the degree of nerve root compression and inform their treatment plan.
Treatment Options for Disc Prolapse
There are many ways to help manage disc prolapse. For most people, treatment starts with conservative steps like physical therapy. This helps strengthen your back muscles and improves your body’s flexibility. This can significantly alleviate symptoms for some people. If you have severe pain or swelling, the use of epidural corticosteroid injections can give fast, short-term help.
If these initial steps are not practical, surgery may be necessary. Doctors may use treatments like discectomy or spinal fusion. These surgeries aim to alleviate nerve root compression and restore the body’s normal functioning. The best approach is to review each person’s case and determine the appropriate course of action based on that.
Conservative and Non-surgical Management
For people who have a disc prolapse, the first things doctors try are non-surgical ways to help with symptoms that can be bad or get in the way of your daily life. Physical therapy is often used, which can help strengthen your back muscles, increase endurance during activity, and improve flexibility. These steps can help alleviate lower back pain and reduce nerve root compression.
Sometimes, the doctor will want you to do special exercises or get epidural corticosteroid injections to help bring down swelling and cut down on pain. All of these methods can help you return to your normal routine, aid in recovery, and prevent further back injuries. This way, you can look forward to less pain and better movement in your lower back.
Surgical Treatments and Procedures
For severe cases of a herniated disc, surgery might be needed to help with pain and get you moving better. There are a few standard procedures for this. In a discectomy, the doctor removes the disc material that is pressing on the nerve root. This helps prevent nerve root compression and associated pain. Another option is a laminectomy. This creates more space in the spinal canal, resulting in less pressure. Sometimes, doctors use spinal fusion to stabilize the spine by joining the bones near the affected area. These types of surgery can help you move more easily and reduce sciatic nerve pain. Most people find it easier to get back to their daily activities with less pain after recovery.
Managing Pain and Discomfort
Dealing with pain and discomfort from disc problems is crucial for a better quality of life. Epidural corticosteroid injections can help reduce swelling around spinal nerves for a short time. Physical therapy helps build muscle strength and improve posture. Engaging in regular exercise tailored to your individual needs can help alleviate back pain and improve your overall mobility. Practicing good ergonomic habits in your daily activities can help alleviate pressure on your back. Everyone is different, so ways to manage pain are discussed together with the doctor. This helps you always feel supported as you heal.
Medications and Injections
The management of disc prolapse uses targeted medicines and injections to help reduce back pain and inflammation. Nonsteroidal anti-inflammatory drugs (NSAIDs) help lessen discomfort from lower back pain and nerve root compression. When pain is very bad, doctors may use epidural corticosteroid injections. These injections work by going straight to the area in the spinal canal that hurts. This way, they address inflammation directly at its source.
This method can make it easier for people to access physical therapy. Physical therapy enhances muscle strength and improves mobility in the lower back. It also helps alleviate leg pain and other issues related to nerve root compression or lower back pain. Being aware of these treatment options empowers people to explore different approaches to recovery.
Physical Therapy and Rehabilitation
Taking part in physical therapy and rehab is very important for recovery from disc prolapse. A program tailored to your needs can help build muscle strength, enhance your mobility, and alleviate pain from herniated discs. People use methods such as manual therapy, specialized exercises, and postural training to restore the spinal cord’s function and relieve pressure on spinal nerves.
Therapists place a lot of emphasis on teaching you how to move in the right way. This helps you perform your daily activities without exacerbating your problem. If you follow the doctor’s rehabilitation plan, you may see improvements in your life, and you can reduce the risk of further injuries.
Prevention and Lifestyle Modifications
Maintaining a healthy body weight and adopting good posture can help reduce the risk of disc prolapse. Engaging in regular exercise, particularly focusing on your back muscles, can improve your muscle strength and help maintain flexibility. This allows your spine a lot. It is also important to consider ergonomics when engaging in your daily activities. When you lift heavy objects or have to sit for long periods, try to set up your work area so that you can maintain a posture that provides your back with good support. Doing some home exercises and stretching can also help prevent problems from worsening. These steps will give you a way to care for your spinal health and lessen the chance of pain from nerve root compression.
Exercise and Posture Correction
Adding targeted exercises to your routine can significantly help ease back pain associated with disc prolapse. When you work on building the strength of your back muscles and core, you give more support to the spine. This can also increase muscle strength, thereby reducing the risk of further disc degeneration. Paying attention to your posture during daily activities is also beneficial. Good posture takes pressure off the nerve root, so you feel less nerve root compression and pain. Gentle stretches and regular exercise can keep your back more flexible. This helps the spine stay healthy. By doing these things, you can feel more comfortable and continue to enjoy an active life.
Ergonomics and Everyday Tips
Creating an ergonomic workspace can significantly alleviate the pain associated with a disc prolapse. When you set your chair to the right height, your feet can rest flat on the floor. This helps you maintain good posture and takes pressure off your lower back. Also, try to take regular breaks during the day. These breaks help prevent your muscles from getting tired and improve blood flow.
If you need to lift heavy objects, be careful with how you do it. Use your legs to lift the weight, not your back, to help avoid injury. Maintaining a healthy body weight is also important. When you do, there is less pressure on the discs in your back, so your lumbar spine can stay healthier.
Conclusion
Understanding disc prolapse is crucial for managing back pain effectively. This problem can make it hard to do your daily activities. It happens when the disc presses on the spinal nerves. This can cause pain and make it tough for you to move. If you get an early diagnosis and the right treatment, you can feel much better. This could be from gentle care or, in some cases, surgery. Engaging in regular exercise, maintaining good posture while sitting and standing, and being aware of risk factors are all helpful in preventing further problems. Taking care of your spine should be a big focus. It helps you live pain-free and allows you to regain your strength and movement.
Consult with top pain specialists in your city.
FAQs
Can a prolapsed disc heal on its own?
A prolapsed disc can get better on its own as time goes on, especially if you take it easy and try things like rest, physical therapy, and ways to help you with pain. However, how quickly you heal can vary from person to person. If you still have problems, you may need to see a doctor for further assistance to recover fully.
What are the warning signs that require immediate medical attention?
You should get medical help right away if you have severe pain, if you feel numbness or weakness in your arms or legs, if you lose control of your bowel or bladder, or if you see an apparent change in how your body looks. These signs can mean you have something serious, like cauda equina syndrome or nerve damage. That is why it is important to get care as soon as possible.
Is disc prolapse the same as a herniated disc?
A herniated disc and disc prolapse are two words that mean almost the same thing. In both cases, the soft inner part of the disc comes out and puts pressure on the spinal nerves. People often use these words for the same problem in the back. However, “prolapse” refers to the disc being out of place, while “herniation” indicates that the outer part of the disc has ruptured.
How long does recovery from disc prolapse take?
Recovery from a disc prolapse can vary for each person. It often takes from a few weeks to several months. The type of treatment you get matters. Your overall health also plays a big part. Sticking to your rehab exercises is also helpful. Talking with a healthcare provider will provide you with personalized advice tailored to your situation and recovery time expectations.
Are there any long-term complications of disc prolapse?
Yes, disc prolapse can lead to long-term problems, including chronic pain, nerve damage, and reduced mobility. In severe cases, individuals may even lose control of their bowel or bladder. To mitigate these risks and improve quality of life, it is essential to receive effective treatment and develop strategies to manage the condition.